|
It can be tempting to think you might be able to self treat a pelvic floor problem. Add in a few kegels to your day and all will be sorted right?
- Not all pelvic floor problems are solved by kegels (doing pelvic floor contraction work), for example: certain pain conditions or tight/hypertonic pelvic floors - If a contraction is appropriate but your technique is wrong, it won't be effective. - Part of pelvic floor rehab is starting at an appropriate level and then progressing appropriately. If you start at the wrong level or don't progress at the right time you may find you don't improve. - It's imperative to make your pelvic floor rehab activity/sport specific to ensure you achieve full resolution of your symptoms during higher lev.el activity Conclusion? Get your GP to refer you to your local NHS physio service or contact your local private pelvic floor physio for a full assessment and treatment.
0 Comments
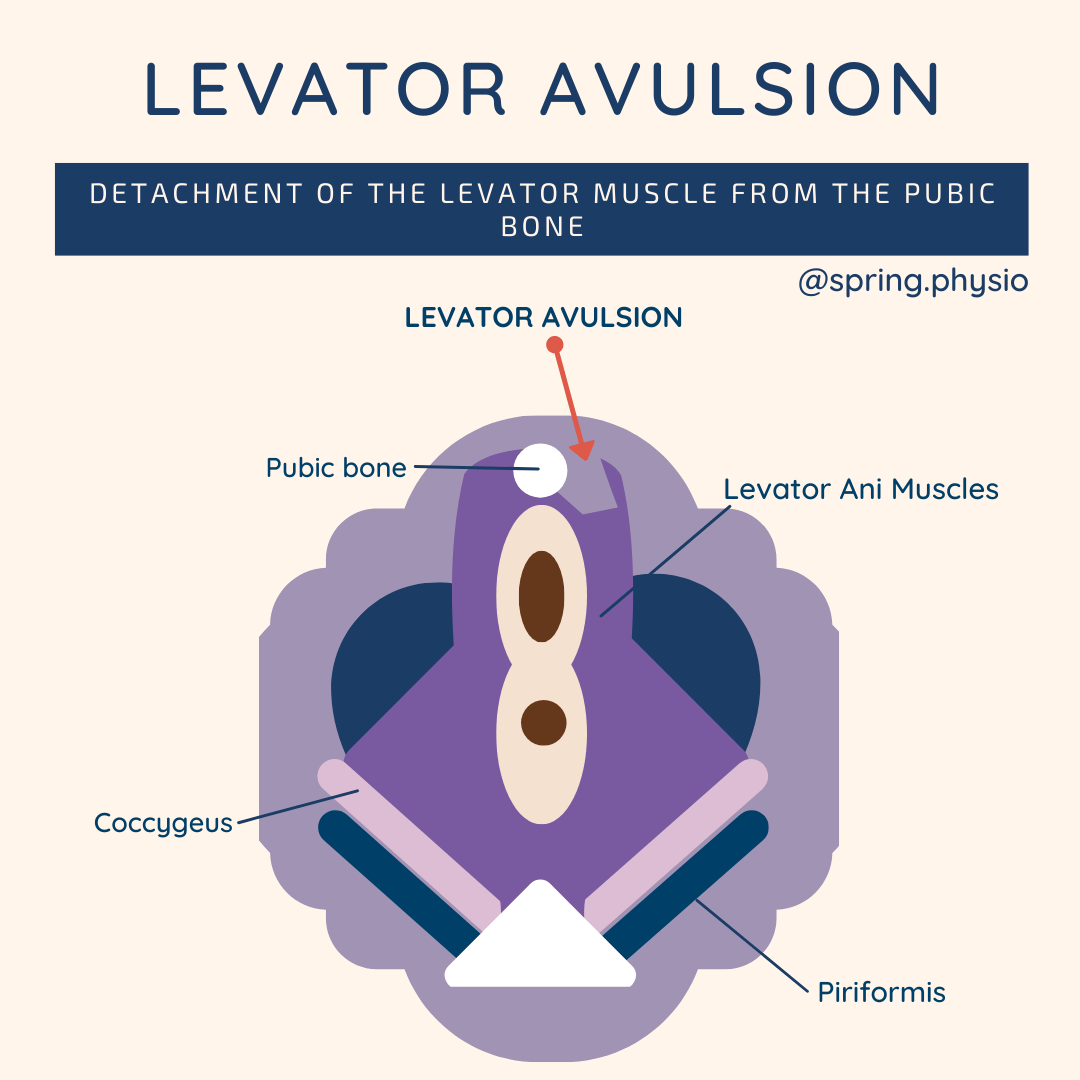
A levator avulsion is where part of the pelvic floor muscles are pulled off the pubic bone. This can affect between 10-35% of women following their first delivery.
The loss of this support can make your pelvic floor weaker, enlarge the opening of the vagina and increase the likelihood of prolapse. A levator injury is not repaired, but if you have been diagnosed with one it makes it even more important to strengthen the intact pelvic muscles - to provide as much support as possible to the pelvic organs. Levator injuries are often not diagnosed immediately but may be picked up by your physiotherapist or gynaecologist during a pelvic examination. Women's health physios do not just teach kegels! And this list is not exhaustive. These are just some of the most common problems I see in my clinic each week.
You can get a referral via your GP for NHS physio or there is a large private network of physios in the UK, which accept self referral. You can book an appointment with our clinic by clicking here I was prompted to share this post because I've had a really nasty bout of coccyx pain recently. However - I've utilised some of these strategies and it's now resolved!
1. Offloading the tailbone is important during sitting. You can buy lots of different ring cushions on amazon but I find the blow up travel neck pillows have worked a treat for me! 2. The pelvic floor can often aggravate or contribute to tailbone pain so pelvic floor stretches can be very helpful in relieving symptoms. 3. Manual therapy doesn't work for everyone but when it does it's great! I then give patients a way of self treating at home. 4. You can try heat or ice, whichever gives relief. I definitely prefer warmth but see what works for you. 5. The coccyx is part of the spine so low back problems can also contribute to tailbone pain. Therefore it is important the spine as a whole is moving freely. Incorporate some spinal mobility exercises into your daily exercise programme. 6. Make sure you are not sitting in a slouched position because this loads the coccyx and can irritate it further. Make sure you're are sitting on your sitting bones (the bony bits in your bottom), not your tailbone!
If your pelvic floor rehab doesn't include some kind of glute strengthening, now is the time to get started! Strong glutes allow your pelvic floor to focus on what it's best at - supporting your pelvic organs and keeping you continent!
I was delighted to produce this infographic for the POGP journal to support Christien Bird's presentation at the POGP conference last year.
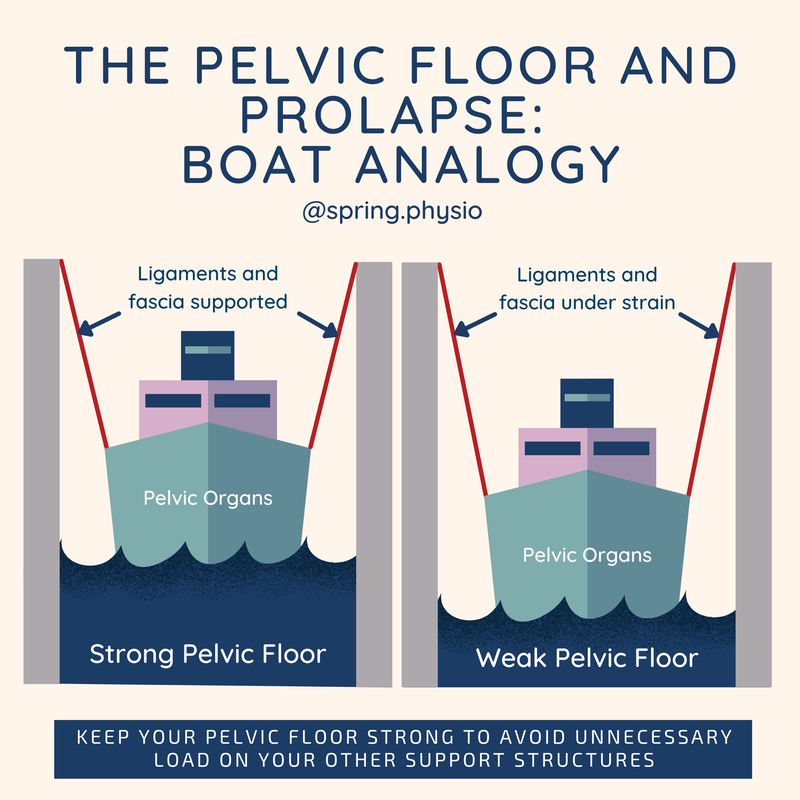
The presentation by Christien covered many different aspects of menopause management but the three key elements that all women need are good sleep, good diet and regular exercise. There is lots of confusing information out there, especially about diet in menopause. But the take home from the presentation was this: Manage your blood sugar levels. The easiest way to do this is through eating a combination of protein and complex carbohydrates. There is a tendency for women to "go to the mat" in the peri/post menopausal years. Whilst there are lots of benefits to doing lower impact mat based exercise, the benefits or doing a mixture of exercise types (including resistance and higher impact) are incredibly important for optimising muscle mass and bone density. Variety is key! The boat in the dock theory (Delancey et al) is a way of illustrating the relationship between the pelvic organs (the boat) pelvic floor (sea), ligaments (ropes) and prolapse.
A weak pelvic floor doesn't cause a prolapse. But over time not having that support puts more strain on the other support systems, which in turn can cause more stretching or damage to the support system. The best approach is to always maintain a strong pelvic floor. If you then stretch or injure any of the connective tissue supports (eg through pregnancy or childbirth), you've still got some solid muscular support. If you've already gott a prolapse and haven't had any pelvic floor strengthening, hopefully you can see from this image why it's so important!
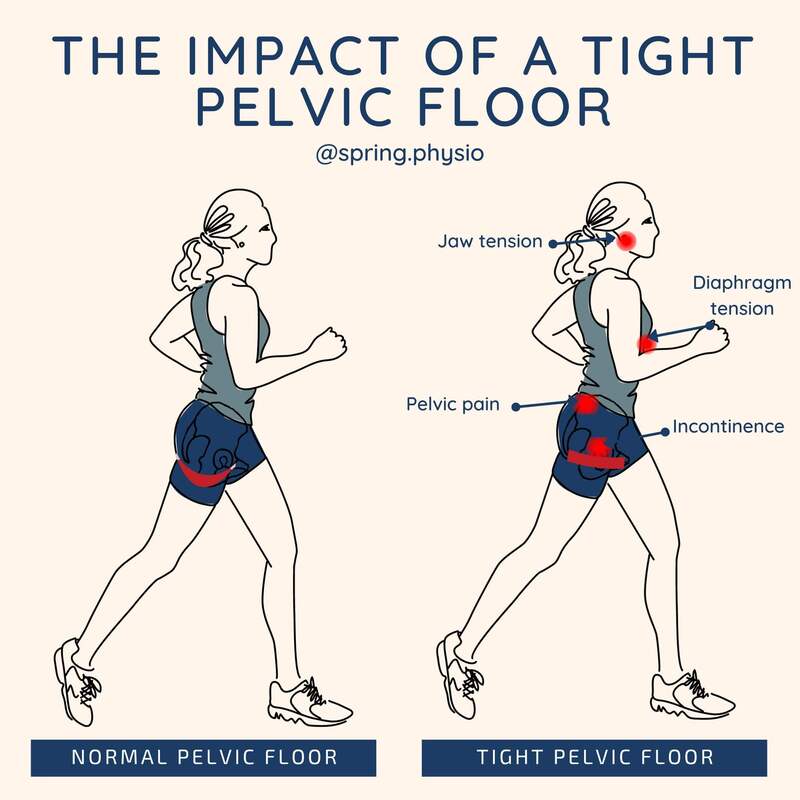
The impact of a tight or hypertonic pelvic floor isn't limited to the pelvis area.
Whist a tight pelvic floor can cause symptoms such as incontinence, painful sex and pelvic pain, the effects can be more far reaching. The pelvic floor is the floor of your core; tightness here will impact other elements of the core system, such as the diaphragm. If the diaphragm becomes tense, this will impact on how optimally the chest expands and contracts with breathing. Our bodies are linked via a support system called fascia. This is connective tissue that runs throughout the body. Because fascia links diffrent areas of the body together, tension in one place can lead to tension in another. For this reason it is not uncommon to experience jaw tension alongside a tight pelvic floor. A tight (hypertonic) pelvic floor can often go undiagnosed because it can present similarly to other pelvic floor problems. Common symptoms include back pain, stress incontinence, urge issues and constipation. These symptoms such as will not improve until the tightness of the muscles is dealt with. For this reason it’s so important to get assessed by a women’s health physio
It can be frustrating when recovery doesn’t go quite to plan. Almost every woman I’ve treated has had at least one blip along the way. Whether it’s increased pain from a c-section, worsening prolapse symptoms or leaking when you have a bad cold, it can be really disheartening. But the thing is, we are not robots! Lack of sleep, nutrition, stress and a change in activity can all cause a flare up of symptoms. But that doesn’t mean all is lost. Keep going on your treatment plan and you will find progress does resume! Sometimes you may find you need to take your rehab level back down a step before increasing it again once your flare up settles.
The NICE guidelines recommend a three month physiotherapy exercise programme for prolapse, because research has found that we need to play the long game! Whilst commitment is required, most women find that a course of physiotherapy is effective to manage their prolapse. |
AuthorClaire is a women's health and sports Physiotherapist. She is the owner of Spring Physio and is based in East Sussex. Archives
April 2024
Categories
All
|







 RSS Feed
RSS Feed